Opioid Addiction Treatment in Nashville, TN
Nashville and communities across Tennessee have been deeply impacted by opioids—prescription painkillers, heroin, and fentanyl. If you or someone you love is struggling, you’re not alone, and effective treatment is available.
Ready for a real next step?
Quick Answer: What treatment works for opioid addiction?
Opioid addiction (also called opioid use disorder/OUD) is treatable. Evidence-based care usually includes:
- Medications for OUD (MOUD) such as buprenorphine, methadone, or naltrexone
- Counseling + behavioral therapies to build coping skills and prevent relapse
- The right level of care (detox, outpatient, PHP, IOP, residential) based on your needs
- Recovery supports + aftercare planning (family involvement, peer support, sober living)
Our role: We help you understand your options, start safely (often beginning with detox when needed), and transition into the level of care that supports long-term recovery.
What is opioid use disorder (OUD)?
OUD is a problematic pattern of opioid use that causes distress and impacts daily life. People sometimes say “opioid dependence” or “opioid addiction.” Dependence can include withdrawal when you stop; addiction includes compulsive use despite harm.
Common opioids include: oxycodone, hydrocodone, codeine, morphine, heroin, and fentanyl.
Signs it may be time to get help:
- You’ve tried to stop but can’t
- Withdrawal symptoms or cravings are driving use
- Relationships, work, or health are suffering
- You’re using more than intended, or in risky situations
Treatment Options We Can Help You Access
Every plan is individualized, but most opioid addiction treatment includes a combination of:
Medications (MOUD)
FDA-approved medications for opioid use disorder include buprenorphine, methadone, and naltrexone.
Therapy and recovery supports
Counseling can help you address triggers, stabilize mental health, and build relapse-prevention skills.
Levels of care
Some people start with detox; others begin in outpatient or structured outpatient depending on safety and withdrawal risk.
Detox vs. treatment: what’s the difference?
Detox is often the first step when your body needs help stabilizing from opioid withdrawal.
Treatment is what helps you stay stable—through medication and withdrawal management (when appropriate), therapy, skills-building, and ongoing support.
If you complete detox but don’t continue care, cravings and relapse risk can remain high. The goal is to build a plan that continues after detox.
Medical Detox For Opioid Withdrawal In Nashville
Our opioid detox approach
Our Nashville-based team supports you through withdrawal with monitoring, comfort-focused care, and clinical guidance.
During detox, you may receive:
- Monitoring and symptom support
- Medications when appropriate to ease withdrawal intensity
- Early recovery planning for what comes next (PHP/IOP/outpatient/residential)
Opioid Withdrawal Symptoms (What You Might Feel)
Opioid withdrawal can be extremely uncomfortable. Symptoms may include anxiety, sweating, nausea, vomiting, diarrhea, muscle aches, insomnia, chills, and agitation.
Important: Everyone’s detox experience is different. A clinical assessment helps determine the safest plan—especially with other substances involved.
How long does opioid detox take?
Many people experience the most intense withdrawal symptoms in the first several days, and detox often lasts around 3–7 days, though this varies by substance, use pattern, and health factors.
After detox, the next step is typically a structured level of care such as PHP (partial hospitalization), depending on your needs.
Medications for opioid addiction (MOUD): what they are and how they differ
Medications can reduce cravings and withdrawal, support recovery, and help lower overdose risk.
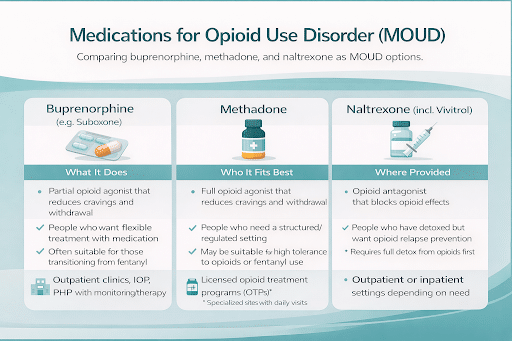
MOUD comparison (quick guide)
Buprenorphine (e.g., Suboxone):
- Partial opioid agonist; helps reduce cravings/withdrawal
- Often used in outpatient settings with monitoring and therapy
Methadone:
- Full opioid agonist, typically provided through regulated opioid treatment programs (OTPs)
- Helpful for some people who need more structured medication support
Naltrexone (including extended-release injection/Vivitrol):
- Opioid antagonist (blocks opioids)
- Often requires being opioid-free for a period before starting (clinician-guided)
What we offer / coordinate
Our MAT approach combines medication support (such as buprenorphine or naltrexone/Vivitrol) with evidence-based therapies.
We do not currently provide methadone on-site, but we can refer you to appropriate providers.
How To Choose The Right Level Of Care (Detox, Php, Iop, Outpatient, Sober Living)
If you need the highest structure…
- Medical Detox (withdrawal stabilization)
- Residential/Inpatient (24/7 structured care through partner facilities, if needed)
If you need structured daytime treatment but sleep at home…
- Partial Hospitalization Program (PHP) (high structure, full/most days)
If you need flexible structure around work/family…
- Intensive Outpatient Program (IOP) (multiple sessions/week)
If you’re stable and need ongoing support…
- Outpatient (less frequent sessions)
Sober Living (recovery housing + accountability)
We’ll explain your options clearly and help you understand what may fit your situation—without pressure.
What To Expect When You Contact Us
When you call (615) 326-6449, our admissions team can help you:
- Understand what’s going on and what you’re using (opioids only vs multiple substances)
- Discuss withdrawal risk and whether detox is needed
- Verify insurance and explain payment options
- Plan next steps (detox → PHP/IOP/outpatient, or partner residential options)
What to have ready (helpful, not required):
- Insurance card (if applicable)
- List of substances used + approximate amounts/frequency
- Current medications and any mental/physical health concerns
Cost Of Opioid Treatment In Nashville + Insurance
The cost of opioid detox services in Nashville can vary widely by setting and length of care. Your current page references a typical range and payment options (insurance/private pay, etc.).
Updated, safer phrasing (recommended):
- We accept many insurance plans and offer private pay options.
- Costs vary based on coverage, clinical needs, and level of care.
The fastest way to understand your cost is to call for a free assessment and insurance verification.
Support for families: how to help someone with opioid addiction
If you’re supporting a loved one:
- Focus on safety and getting a clinical assessment
- Avoid arguments during intoxication/withdrawal
- Set boundaries and offer a clear next step (call together)
- Consider family programming and therapy
You can call us even if your loved one isn’t ready yet: (615) 326-6449
Resources: Help In Nashville And Beyond
- SAMHSA National Helpline: 1-800-662-HELP (4357), free/confidential 24/7
- FindTreatment.gov (treatment locator)
- Southeast Addiction Center Tennessee is a Nashville-based rehab center that provides outpatient detox and Medication-Assisted Treatment as well as inpatient detox through its partner facilities. Call us 24/7 for help.
- Tennessee Recovery Navigators is a non-profit organization that offers peer-based recovery support services, including opioid detox resources. They provide support to individuals in their journey to recovery, offering resources for detox, counseling, and aftercare.
- The Tennessee Department of Mental Health and Substance Abuse provides a variety of services to individuals in the Nashville area, including a directory of MAT addiction treatment providers.
Nashville CARES is a well-known organization in Nashville that provides a variety of services to individuals in the area, including counseling and recovery support services. They provide individuals with the resources they need to successfully navigate the recovery process. Overall, there are a variety of organizations in Nashville that provide opioid detox services to individuals struggling with addiction. With the help of these organizations, individuals can access resources to help them in their journey to recovery.
Our Programs
- Partial Hospitalization Program (PHP)
- Intensive Outpatient Program (IOP)
- Medical Detox
- Sober Living
About Us
- Our Team
- Tour
- Testimonials
- FAQs
Your Recovery Starts Here
Our admissions team is ready 24/7 to guide you through the process, from admission to coordinating travel, treatment programs, and more.
Most Insurances Accepted










Opioid Addiction Treatment FAQs

Evidence-based treatment often includes MOUD + counseling/behavioral therapy and the right level of care.
FDA-approved medications include buprenorphine, methadone, and naltrexone.
Buprenorphine is an evidence-based treatment used to reduce cravings/withdrawal and support recovery under medical supervision.
Detox duration varies; many people stabilize within about a week, but needs differ.
Not always. A clinical assessment determines whether detox is necessary or if you can start treatment in outpatient/PHP/IOP.
Yes—fentanyl is an opioid, and treatment options may include detox, MOUD, therapy, and structured levels of care.
Many people step into PHP, IOP, outpatient, sober living, or residential care depending on stability and support needs.
Call us—availability depends on clinical needs and program capacity, but we’ll move quickly to help you find the right next step.
Yes. Family therapy and support can be part of treatment planning.
Relapse can be part of the recovery process for some people. The priority is safety and returning to care quickly.